Reducing Avoidable Hospital Admissions and A&E Attendances with Technology that Strengthens Integrated Neighbourhood Teams (INTs)
Avoidable hospital admissions and A&E attendances remain a major challenge across the NHS, particularly for people living with frailty. These admissions are often driven by fragmented care, poor continuity, and a lack of coordinated action across teams.
THS enables Integrated Neighbourhood Teams (INTs) to take a proactive, population health approach, improving outcomes for older people and reducing avoidable A&E use. This is delivering sustained reductions in attendances for people aged 75 and over, with even greater impact in care homes.
Find out more below.
Population Health Management starts with identification.
Accurate Frailty identification matters.
Half of all hospital beds in the UK are occupied by people aged 75 or more. Most have frailty.
Superior diagnostic accuracy
Compared with eFI 1, it identified twice as many people at high risk of frailty, with clinicians confirming frailty in 75.9%.
Systematically screens all over 65s
Every year the Pathfields Tool screens all over-65s with high-risk features. If a clinician opens their notes, it prompts a frailty diagnosis. Once completed, it stays dormant for a year.
Identifies mild frailty
Systematic detection of mild frailty, enabling earlier intervention, slowing decline, and in some cases preventing progression altogether
Evidence based
The Pathfields Tool, which has been independently peer reviewed and published.
Time neutral
Unlike other tools, this is time neutral. Diagnosis relies on the clinician’s knowledge of the patient and two clicks of a mouse button.
The Pathfields Tool. Superior frailty identification built for real clinical practice.

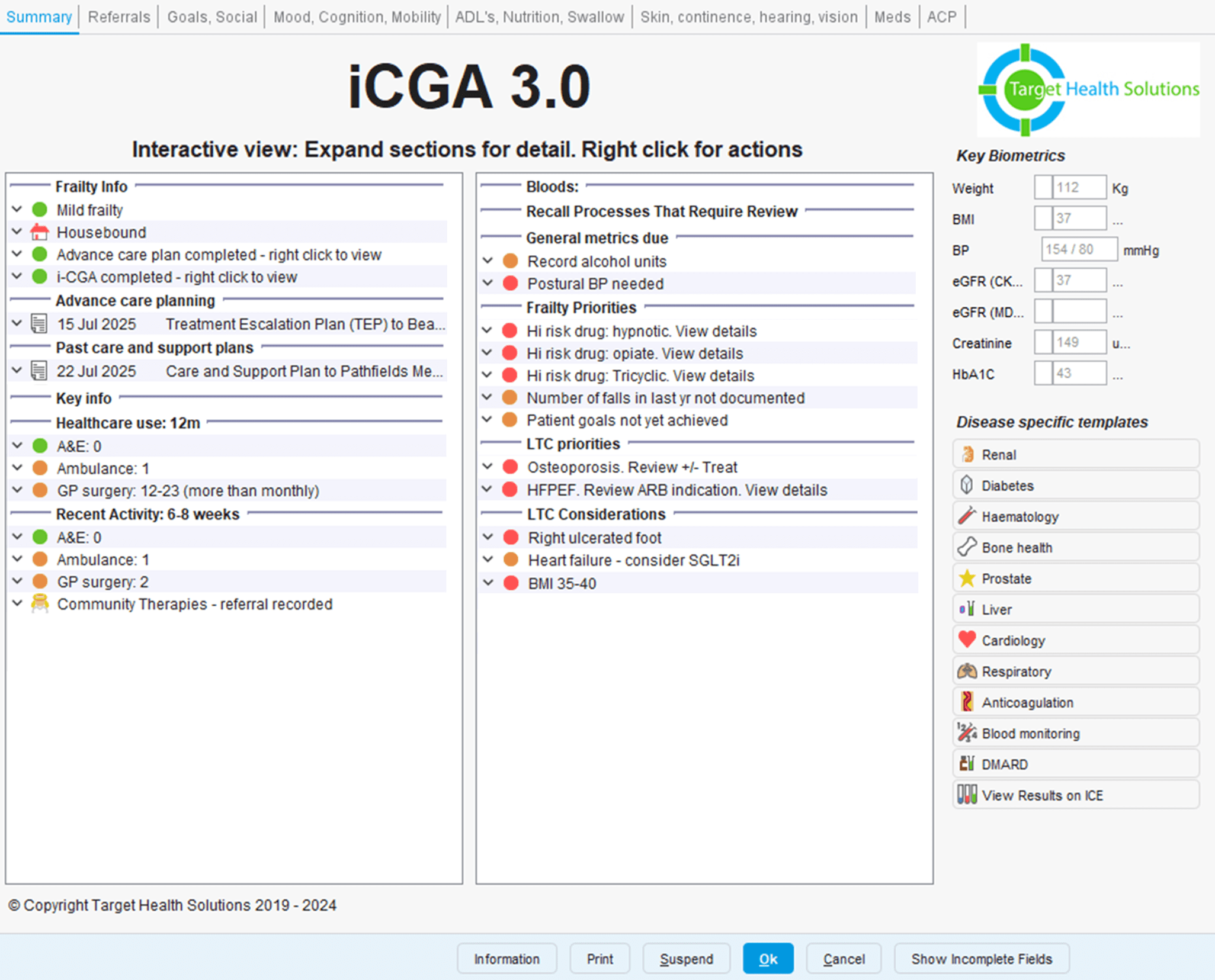
Population Health Management ends with iCGA 3.0 powering Integrated Neighbourhood Teams (INTs).
One Team. One assessment.
Healthcare useage
iCGA 3.0 shows which services a patient has been known to in the last six to twelve months and their healthcare use over the past six to eight weeks.
This helps teams spot early signs of an evolving crisis.
At a glance view
A rapid overview of the person’s frailty status, care setting, advance care planning preferences, and link to their latest care and support plan.
Superior automated recalls
It saves time, cuts workload, and ensures nothing is missed.
Recalls can be tailored so people with complex needs are seen more often until things improve.
IT-assisted decision support
This strengthens clinical decision making, upskills the workforce, and ensures every iCGA is thorough and consistent.
Greater efficiency
Most actions are automated, including creating and sharing the care and support plan. Duplication has also been eliminated, giving clinicians more time to focus on patient care.
Continuity with one single source of truth
iCGA improves continuity by giving all teams one shared, accurate record.
Care and support plans are generated and shared instantly with the patient and every organisation in the Integrated Neighbourhood Team (INT), so everyone works from the same information when the patient needs help.
Evidence based
iCGA 3.0 is a third generation, IT-assisted CGA with enhanced decision support. Its earlier version, iCGA 2, has been independently peer reviewed, published, and shown to improve survival.
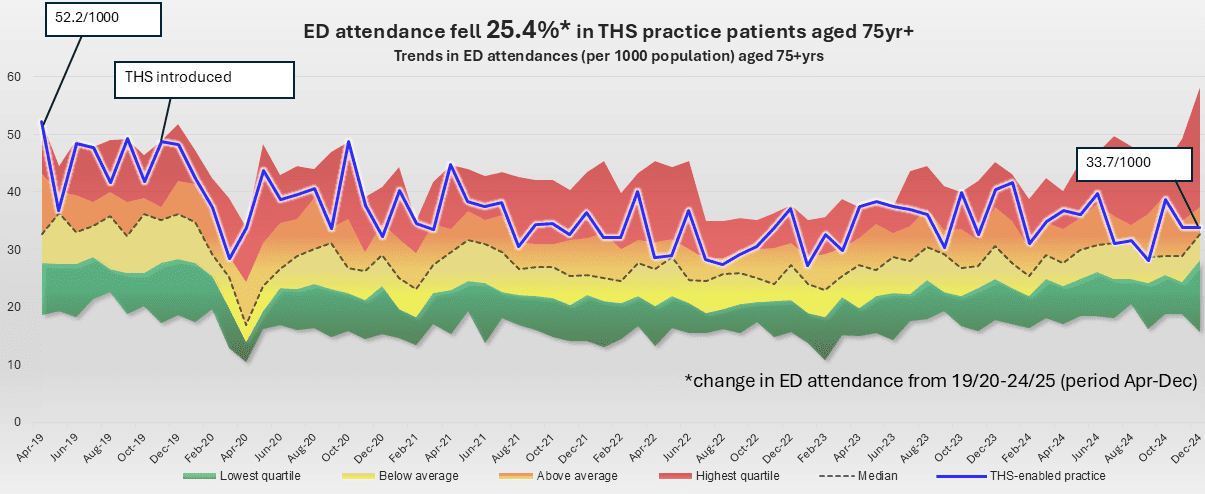
What's the impact?
Other benefits
Reduced A&E attendance from care homes
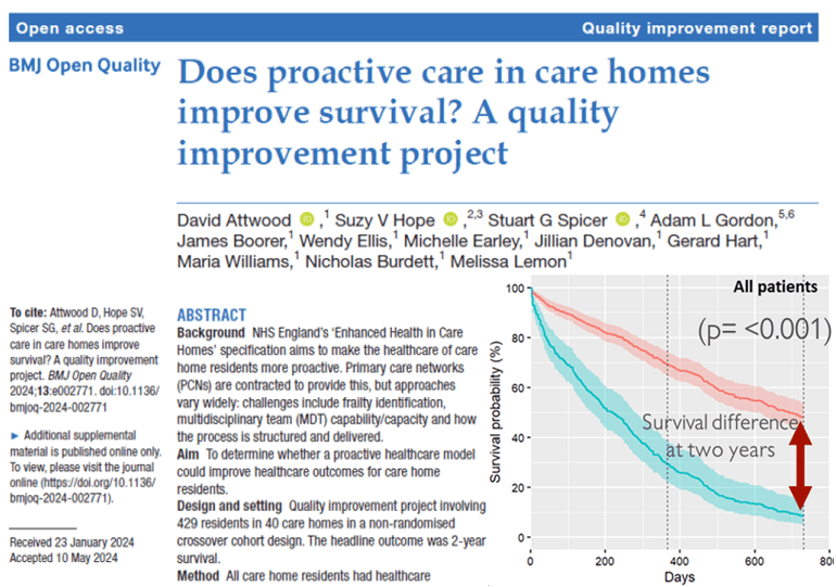
Living longer
Independent research found that proactive care and iCGA improved two-year survival by 39.6 percent in a study of 429 care home residents, compared with routine NHS care.
Living better
Reduced A&E attendance from care homes
Living longer
Independent research found that proactive care and iCGA improved two-year survival by 39.6 percent in a study of 429 care home residents, compared with routine NHS care.
Living better
This is just the beginning.
Automating Great Care
Target Health Solutions helps GP practices deliver better care more efficiently, leading to improved patient outcomes, increased QOF income, greater productivity and increased profit.


Book a Demo